48 results
I don’t know where I’m going or where I come from. Self-disorders in schizophrenia.
- M. D. C. Vallecillo Adame, L. Rodríguez Andrés, C. de Andrés Lobo, T. Jimenez Aparicio, M. Queipo de Llano de la Viuda, G. Guerra Valera, A. A. Gonzaga Ramirez, M. Fernández Lozano, M. J. Mateos Sexmero, N. Navarro Barriga, B. Rodríguez Rodríguez, M. P. Pando Fernández, M. Calvo Valcárcel, P. Martínez Gimeno, M. A. Andreo Vidal, I. D. L. M. Santos Carrasco
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S1069-S1070
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
In the early stages of schizophrenia the person experiences feelings of strangeness about themselves, difficulty in making sense of things and difficulty in interacting with their environment. Based on this, self-disorder assessment instruments have been developed and empirical studies have been conducted to assess people at risk of developing a schizophrenia spectrum disorder. These studies show that self-disorders are found in pre-psychotic stages and that their manifestation can predict the transition to schizophrenia spectrum disorders.
ObjectivesWe present the case of a patient with multiple diagnoses and mainly dissociative symptoms who, after years of evolution, was diagnosed with schizophrenia.
MethodsBibliographic review including the latest articles in Pubmed about self-disorders and schizophrenia.
ResultsWe present the clinical case of a 51-year-old woman with a long history of follow-up in mental health consultations and with multiple hospital admissions to the psychiatric unit, with several diagnoses including: dissociative disorder, histrionic personality disorder, adaptive disorder unspecified psychotic disorder and, finally, schizophrenia. The patient during the first hospital admissions showed a clinical picture of intense anxiety, disorientation and claiming to be a different person. The patient related these episodes to stressors she had experienced, and they improved markedly after a short period of hospital admission. Later, psychotic symptoms appeared in the form of auditory and visual hallucinations and delusional ideation, mainly of harm, so that after several years of follow-up and study in mental health consultations and in the psychiatric day hospital, she was diagnosed with schizophrenia and treatment with antipsychotics was introduced, with a marked clinical improvement being observed.
ConclusionsIt is important to take into account this type of symptoms (self-disorders), as they allow the identification of individuals in the early stages of the disorder and create the opportunity for early therapeutic interventions.
Disclosure of InterestNone Declared
Relationship between CAINS negative symptoms and cognition, psychosocial functioning and quality of life in patients with a first psychotic episode of schizophrenia
- R. Rodriguez-Jimenez, L. García-Fernández, V. Romero-Ferreiro, M. Valtueña García, A. I. Aparicio, J. M. Espejo-Saavedra, L. Sánchez-Pastor, A. Nuñez-Doyle, M. Dompablo, O. Jiménez-Rodríguez, D. Rentero, P. Fernández-Sotos, I. Martínez-Gras, J. L. Santos
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S641-S642
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Negative symptoms has been classically associated with cognition, psychosocial functioning and quality of life in patients with schizophrenia. But negative symptoms are not a unitary construct, encompassing two different factors: diminished expression, and motivation and pleasure. Few works have studied the relationship between these two different negative symptoms factors and cognition (neuro and social cognition), psychosocial functioning and quality of life, jointly, in patients with a first psychotic episode of schizophrenia.
ObjectivesThe objective of the present work was to study, in a sample of patients with a first psychotic episode of schizophrenia, the relationship between the negative symptoms (diminished expression and motivation and pleasure) and neurocognition, social cognition, functioning and quality of life.
MethodsThe study was carried out with 82 outpatients with a first psychotic episode of schizophrenia from two Spanish hospitals (“12 de Octubre” University Hospital, Madrid and “Virgen de la Luz” Hospital, Cuenca). The patients were assessed with the Clinical Assessment Interview for Negative Symptoms (CAINS) for evaluating diminished expression (EXP) and motivation and pleasure (MAP) symptoms, the MATRICS Consensus Cognitive Battery (MCCB) for evaluating neurocognition and social cognition, the Social and Occupational Functioning Assessment Scale (SOFAS), and the Quality of Life Scale (QLS).
ResultsA negative correlation was found between neurocognition and the two negative symptoms subscales: CAINS-EXP (r=-0.458, p<0.001) and CAINS-MAP (r=-0.374, p<0.001); but with social cognition only CAINS-EXP was correlated (r=-0.236, p=0.033). Also, it was found a high negative correlation between SOFAS scores and CAINS-MAP (r=-0.717, p<0.001); and a medium negative correlation with CAINS-EXP (r=-0.394, p<0.001). Finally, QLS score was high correlated with both CAINS subscales: CAINS-EXP (r=-0.681, p<0.001) and CAINS-MAP (r=-0.770, p<0.001).
ConclusionsThis study found a relationship between negative symptoms and neurocognition, social cognition, functioning and quality of life in a sample of patients with a first psychotic episode of schizophrenia. But the two different negative symptom factors, diminished expression, and motivation and pleasure, are associated differently with psychosocial functioning, but especially with social cognition where the relationship was only found with diminished expression symptoms.
Disclosure of InterestNone Declared
Late diagnosis of attention deficit hyperactivity disorder and cocaine abuse
- C. De Andrés Lobo, C. Vallecillo Adame, T. Jiménez Aparicio, M. Queipo de Llano de la Viuda, G. Guerra Valera, A. A. Gonzaga Ramírez, M. Fernández Lozano, N. Navarro Barriga, M. J. Mateos Sexmero, B. Rodríguez Rodríguez, M. Calvo Valcárcel, M. Andreo Vidal, M. P. Pando Fernández, P. Martínez Gimeno, I. D. L. M. Santos Carrasco, J. I. Gonçalves Cerejeira, A. Rodríguez Campos
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S335-S336
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Adult ADHD diagnosis sometimes represents a challenge for the clinician, due to the comorbid psychiatric diseases that are often associated and which complicate de recognition of the primary symptoms of ADHD. The prevalence of ADHD in adult populations is 2’5% and it is a relevant cause of functional impairment.
ObjectivesPresentation of a clinical case of a male cocaine user diagnosed with adult ADHD.
MethodsLiterature review on adult ADHD and comorbid substance abuse.
ResultsA 43-year-old male who consulted in the Emergency Department due to auditory hallucinosis in the context of an increase in his daily cocaine use. There were not delusional symptoms associated and judgment of reality was preserved. Treatment with olanzapine was started and the patient was referred for consultation. In psychiatry consultations, he did not refer sensory-perceptual alterations anymore, nor appeared any signals to suspect so, and he was willing to abandon cocaine use after a few appointments. He expressed some work concerns, highlighting that in recent months, in the context of a greater workload, he had been given several traffic tickets for “distractions.” His wife explained that he had always been a inattentive person (he forgets important dates or appointments) and impulsive, sometimes interrupting conversations. In the Barkley Adult ADHD Rating Scale he scored 32 points.
He was diagnosed with adult ADHD and treatment with extended-release methylphenidate was started with good tolerance and evolution, with improvement in adaptation to his job and social environment. Since then, the patient has moderately reduced the consumption of drugs, although he continues to use cocaine very sporadically.
ConclusionsEarly detection of ADHD and its comorbidities has the potential to change the course of the disorder and the morbidity that will occur later in adults. Comorbidity in adult ADHD is rather the norm than the exception, and it renders diagnosis more difficult. The most frequent comorbidities are usually mood disorders, substance use disorders, and personality disorders. Treatment of adult ADHD consists mainly of pharmacotherapy supported by behavioral interventions. When ADHD coexists with another disorder, the one that most compromises functionality will be treated first and they can be treated simultaneously. The individual characteristics of each patient must be taken into account to choose the optimal treatment.
Disclosure of InterestNone Declared
“The cat and the calcium”. A case of delirium secondary to hypercalcaemia.
- T. Jiménez Aparicio, C. Vallecillo Adame, C. de Andrés Lobo, G. Medina Ojeda, M. Queipo de Llano de la Viuda, A. A. Gonzaga Ramírez, G. Guerra Valera, M. Fernández Lozano, M. J. Mateos Sexmero, B. Rodríguez Rodríguez, N. Navarro Barriga, M. A. Andreo Vidal, M. Calvo Valcárcel, P. Martínez Gimeno, M. P. Pando Fernández, I. D. L. M. Santos Carrasco, J. I. Gonçalves Cerejeira
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S946-S947
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Interconsultation with the psychiatry service is frequently requested from other specialties for the assessment and treatment of patients who present neuropsychiatric symptoms secondary to organic alterations. On the other hand (and in relation to this case), within the possible causes for the elevation of calcaemia figures, the most frequent are hyperparathyroidism and neoplasms, representing between these two entities 90% of cases (1).
Among the organic mental disorders, Delirium stands out, with an approximate prevalence between 1 and 2% (general population), which increases in hospitalized and elderly patients (2).
ObjectivesPresentation of a clinical case about a patient with delirium secondary to hypercalcemia, with hallucinations and behavioral disturbance.
MethodsBibliographic review including the latest articles in Pubmed about delirium (causes and treatment) and hypercalcaemia secondary to neoplasms.
ResultsWe present a 52-year-old male patient, who went to the emergency room accompanied by his wife, due to behavioral alteration. Two days before, he had been evaluated by Neurology, after a first epileptic crisis (with no previous history) that resolved spontaneously. At that time, it was decided not to start antiepileptic treatment.
The patient reported that he had left his house at midnight, looking for a cat. As he explained, this cat had appeared in his house and had left his entire bed full of insects. His wife denied that this had really happened, and when she told the patient to go to the emergency room, he had become very upset.
As background, the patient used to consume alcohol regularly, so the first hypothesis was that this was a withdrawal syndrome. However, although the consumption was daily, in recent months it was not very high, and at that time no other symptoms compatible with alcohol withdrawal were observed (tremor, tachycardia, sweating, hypertension…).
We requested a general blood test and a brain scan. The only relevant finding was hypercalcaemia 12.9mg/dL (which could also be the origin of the previous seizure). It was decided to start treatment with Diazepam and Tiapride in the emergency room, with serum perfusion, and keep under observation. After several hours, the patient felt better, the hallucinations disappeared, and calcium had dropped to 10.2mg/dL. A preferential consultation was scheduled, due to suspicion that the hypercalcaemia could be secondary to a tumor process.
Image:
 Conclusions
ConclusionsIt is important to rule out an organic alteration in those patients who present acute psychiatric symptoms. Hypercalcaemia is frequently associated with tumor processes (1) due to secretion of PTH-like peptide (4), so a complete study should be carried out in these cases.
Delirium has a prevalence between 1 and 2% in the general population (2).
Psychopharmacological treatment is used symptomatically, with antipsychotics (3). For the episode to fully resolve, the underlying cause must be treated.
Disclosure of InterestNone Declared
Cannabis use as a potential mediator between childhood adversity and first-episode psychosis: results from the EU-GEI case–control study
- Giulia Trotta, Victoria Rodriguez, Diego Quattrone, Edoardo Spinazzola, Giada Tripoli, Charlotte Gayer-Anderson, Tom P Freeman, Hannah E Jongsma, Lucia Sideli, Monica Aas, Simona A Stilo, Caterina La Cascia, Laura Ferraro, Daniele La Barbera, Antonio Lasalvia, Sarah Tosato, Ilaria Tarricone, Giuseppe D'Andrea, Andrea Tortelli, Franck Schürhoff, Andrei Szöke, Baptiste Pignon, Jean-Paul Selten, Eva Velthorst, Lieuwe de Haan, Pierre-Michel Llorca, Paulo Rossi Menezes, Cristina M Del Ben, Jose Luis Santos, Manuel Arrojo, Julio Bobes, Julio Sanjuán, Miquel Bernardo, Celso Arango, James B Kirkbride, Peter B Jones, Alexander Richards, Bart P Rutten, Jim Van Os, Isabelle Austin-Zimmerman, Zhikun Li, Craig Morgan, Pak C Sham, Evangelos Vassos, Chloe Wong, Richard Bentall, Helen L Fisher, Robin M Murray, Luis Alameda, Marta Di Forti, EU-GEI WP2 Group
-
- Journal:
- Psychological Medicine / Volume 53 / Issue 15 / November 2023
- Published online by Cambridge University Press:
- 04 May 2023, pp. 7375-7384
-
- Article
-
- You have access Access
- Open access
- HTML
- Export citation
-
Background
Childhood adversity and cannabis use are considered independent risk factors for psychosis, but whether different patterns of cannabis use may be acting as mediator between adversity and psychotic disorders has not yet been explored. The aim of this study is to examine whether cannabis use mediates the relationship between childhood adversity and psychosis.
MethodsData were utilised on 881 first-episode psychosis patients and 1231 controls from the European network of national schizophrenia networks studying Gene–Environment Interactions (EU-GEI) study. Detailed history of cannabis use was collected with the Cannabis Experience Questionnaire. The Childhood Experience of Care and Abuse Questionnaire was used to assess exposure to household discord, sexual, physical or emotional abuse and bullying in two periods: early (0–11 years), and late (12–17 years). A path decomposition method was used to analyse whether the association between childhood adversity and psychosis was mediated by (1) lifetime cannabis use, (2) cannabis potency and (3) frequency of use.
ResultsThe association between household discord and psychosis was partially mediated by lifetime use of cannabis (indirect effect coef. 0.078, s.e. 0.022, 17%), its potency (indirect effect coef. 0.059, s.e. 0.018, 14%) and by frequency (indirect effect coef. 0.117, s.e. 0.038, 29%). Similar findings were obtained when analyses were restricted to early exposure to household discord.
ConclusionsHarmful patterns of cannabis use mediated the association between specific childhood adversities, like household discord, with later psychosis. Children exposed to particularly challenging environments in their household could benefit from psychosocial interventions aimed at preventing cannabis misuse.
Tobacco use in first-episode psychosis, a multinational EU-GEI study
- T. Sánchez-Gutiérrez, E. Rodríguez-Toscano, L. Roldán, L. Ferraro, M. Parellada, A. Calvo, G. López, M. Rapado-Castro, D. La Barbera, C. La Cascia, G. Tripoli, M. Di Forti, R. M. Murray, D. Quattrone, C. Morgan, J. van Os, P. García-Portilla, S. Al-Halabí, J. Bobes, L. de Haan, M. Bernardo, J. L. Santos, J. Sanjuán, M. Arrojo, A. Ferchiou, A. Szoke, B. P. Rutten, S. Stilo, G. D'Andrea, I. Tarricone, EU-GEI WP2 Group, C. M. Díaz-Caneja, C. Arango
-
- Journal:
- Psychological Medicine / Volume 53 / Issue 15 / November 2023
- Published online by Cambridge University Press:
- 26 April 2023, pp. 7265-7276
-
- Article
- Export citation
-
Background
Tobacco is a highly prevalent substance of abuse in patients with psychosis. Previous studies have reported an association between tobacco use and schizophrenia. The aim of this study was to analyze the relationship between tobacco use and first-episode psychosis (FEP), age at onset of psychosis, and specific diagnosis of psychosis.
MethodsThe sample consisted of 1105 FEP patients and 1355 controls from the European Network of National Schizophrenia Networks Studying Gene–Environment Interactions (EU-GEI) study. We assessed substance use with the Tobacco and Alcohol Questionnaire and performed a series of regression analyses using case-control status, age of onset of psychosis, and diagnosis as outcomes and tobacco use and frequency of tobacco use as predictors. Analyses were adjusted for sociodemographic characteristics, alcohol, and cannabis use.
ResultsAfter controlling for cannabis use, FEP patients were 2.6 times more likely to use tobacco [p ⩽ 0.001; adjusted odds ratio (AOR) 2.6; 95% confidence interval (CI) [2.1–3.2]] and 1.7 times more likely to smoke 20 or more cigarettes a day (p = 0.003; AOR 1.7; 95% CI [1.2–2.4]) than controls. Tobacco use was associated with an earlier age at psychosis onset (β = −2.3; p ⩽ 0.001; 95% CI [−3.7 to −0.9]) and was 1.3 times more frequent in FEP patients with a diagnosis of schizophrenia than in other diagnoses of psychosis (AOR 1.3; 95% CI [1.0–1.8]); however, these results were no longer significant after controlling for cannabis use.
ConclusionsTobacco and heavy-tobacco use are associated with increased odds of FEP. These findings further support the relevance of tobacco prevention in young populations.
High-fat diet consumption by male rat offspring of obese mothers exacerbates adipose tissue hypertrophy and metabolic alterations in adult life
- Guadalupe L. Rodríguez-González, Sergio De Los Santos, Dayana Méndez-Sánchez, Luis A. Reyes-Castro, Carlos A. Ibáñez, Patricia Canto, Elena Zambrano
-
- Journal:
- British Journal of Nutrition / Volume 130 / Issue 5 / 14 September 2023
- Published online by Cambridge University Press:
- 22 November 2022, pp. 783-792
- Print publication:
- 14 September 2023
-
- Article
- Export citation
-
Obese mothers’ offspring develop obesity and metabolic alterations in adulthood. Poor postnatal dietary patterns also contribute to obesity and its comorbidities. We aimed to determine whether in obese mothers’ offspring an adverse postnatal environment, such as high-fat diet (HFD) consumption (second hit) exacerbates body fat accumulation, metabolic alterations and adipocyte size distribution. Female Wistar rats ate chow (C-5 %-fat) or HFD (maternal obesity (MO)-25 %-fat) from weaning until the end of lactation. Male offspring were weaned on either control (C/C and MO/C, maternal diet/offspring diet) or HFD (C/HF and MO/HF) diet. At 110 postnatal days, offspring were killed. Fat depots were excised to estimate adiposity index (AI). Serum glucose, triglyceride, leptin, insulin, insulin resistance index (HOMA-IR), corticosterone and dehydroepiandrosterone (DHEA) were determined. Adipocyte size distribution was evaluated in retroperitoneal fat. Body weight was similar in C/C and MO/C but higher in C/HF and MO/HF. AI, leptin, insulin and HOMA-IR were higher in MO/C and C/HF v. C/C but lower than MO/HF. Glucose increased in MO/HF v. MO/C. C/HF and MO/C had higher triglyceride and corticosterone than C/C, but lower corticosterone than MO/HF. DHEA and the DHEA/corticosterone ratio were lower in C/HF and MO/C v. C/C, but higher than MO/HF. Small adipocyte proportion decreased while large adipocyte proportions increased in MO/C and C/HF v. C/C and exacerbated in MO/HF v. C/HF. Postnatal consumption of a HFD by the offspring of obese mothers exacerbates body fat accumulation as well as the decrease of small and the increase of large adipocytes, which leads to larger metabolic abnormalities.
Significant early and long-term improvement of neuropsychiatry symptomatology in HCV-infected patients after viral eradication with DAA
- R. Martin-Santos, C. Bartrés, L. Nacar, R. Navinés, M. Cavero, S. Lens, S. Rodriguez-Tajes, J.C. Pariante, I. Horrillo, E. Muñoz-Moreno, N. Bargallo, L. Capuron, J. Meana, X. Forns, Z. Mariño
-
- Journal:
- European Psychiatry / Volume 65 / Issue S1 / June 2022
- Published online by Cambridge University Press:
- 01 September 2022, pp. S238-S239
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Chronic Hepatitis C infection is considered a systemic disease with extrahepatic manifestations, mainly neuropsychiatric symptoms, which is associated with a chronic low-grade inflammatory state. Hepatitis C virus (HCV) eradication is currently achieved in >98% of cases with oral direct-acting antivirals (DAA).
ObjectivesTo study potential clinical neuropsychiatric changes (mood, cognition, sleep, gastrointestinal, sickness, and motion) in HCV-infected patients after HCV eradication with DAA.
MethodsDesign: Cohort study. Subjects: 37 HCV-infected patients, aged<55 years old, with non-advanced liver disease receiving DAA; free of current mental disorder. 24 healthy controls were included at baseline. Assessment: -Baseline (BL) (socio-demographic and clinical variables, MINI-DSM-IV, and Neurotoxicity Scale (NRS), (mood, cognitive, sleep, gastrointestinal, sickness and motor dimensions). Follow-up: End-of-treatment, 12weeks-after and 48weeks-after DAA: NRS. Analysis: Descriptive and bivariate non-parametrical analysis.
ResultsNRS total score and dimensions where different between cases and controls (.000) at baseline. NRS total score (.000) and mood (.000), cognition (.000), sleep (.002), gastrointestinal (.017), and sickness (.003), except motor dimension score (.130) showed significant longitudinal improvement.
ConclusionsHCV-infected patients with mild liver disease presented significantly worse scores for neurotoxicity symptomatology in all dimensions compared to healthy individuals. After HCV eradication with DAA, both at short and long follow-up a significant improvement of the NRS total score and each of the dimensions (except motor) were observed. However, they did not reach the values of healthy individuals, suggesting a not complete neuropsychiatric restoration in the period studied. Grant: ICIII-FIS:PI17/02297.(One way to make Europe) (RMS) and Gilead Fellowship-GLD17/00273 (ZM); and the support of SGR17/1798 (RMS)
DisclosureNo significant relationships.
Mutism. What to expect?
- I. Santos Carrasco, J. Gonçalves Cerejeira, M. Fernández Lozano, A. Gonzaga Ramírez, M. Queipo De Llano De La Viuda, G. Guerra Valera, C. Vallecillo Adame, C. De Andrés Lobo, T. Jiménez Aparicio, B. Rodríguez Rodríguez, N. Navarro Barriga, M.J. Mateos Sexmero, E. Pérez, L. Gallardo Borge
-
- Journal:
- European Psychiatry / Volume 65 / Issue S1 / June 2022
- Published online by Cambridge University Press:
- 01 September 2022, p. S588
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Mutism is the inability or unwillingness to speak, resulting in an absence or marked paucity of verbal output. Mutism is a common manifestation of psychiatric, neurological, and drug-related illnesses. Psychiatric disorders associated with mutism include schizophrenia, affective disorders, conversion reactions, dissociative states, and dementias. Neurological disorders causing mutism affect the basal ganglia, frontal lobes, or the limbic system.
ObjectivesOutline the importance of setting a differential diagnosis of mutism in the Emergency Room.
MethodsReview of scientific literature based on a relevant clinical case.
ResultsMale, 58 years old. He has lived in a residence for 3 months due to voluntary refusal to ingest. Diagnosed with paranoid personality disorder. He is refered to the Emergency Service due to sudden mutism. During this day, he has been stable and suitable with a good functionality. For 3 hours he is mutist, oppositional attitude and stiff limbs, refusing to obey simple orders. Hyperalert and hyperproxia. Not staring. After ruling out organic pathology: normal blood tests, negative urine toxins and cranial CT without alterations, he was admitted to Psychiatry for observation and, finally, he was diagnosed with Psychotic Disorder NOS.
ConclusionsMutism most often occurs in association with other disturbances in behavior, thought processes, affect, or level of consciousness. The most common disorder of behavior occurring with mutism is catatonia. The differential diagnosis of mutism is complex. In some cases the diagnosis will be clarified only by careful observation and after a neurological evaluation. Published studies show neurological disorders presenting with mutism can be misdiagnosed as psychiatric.
DisclosureNo significant relationships.
Personality disorders and Juvenil Myoclonic Epilepsy
- I. Santos Carrasco, J. Gonçalves Cerejeira, M. Queipo De Llano De La Viuda, A. Gonzaga Ramírez, G. Guerra Valera, T. Jiménez Aparicio, C. De Andrés Lobo, C. Vallecillo Adame, M. Fernández Lozano, B. Rodríguez Rodríguez, N. Navarro Barriga, M.J. Mateos Sexmero, L. Gallardo Borge
-
- Journal:
- European Psychiatry / Volume 65 / Issue S1 / June 2022
- Published online by Cambridge University Press:
- 01 September 2022, p. S668
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
There is a high comorbidity between psychiatric disorders and juvenile myoclonic epilepsy (JME), observed in up to 58% of these patients; specifically, mood disorders, anxiety and personality disorders (PD). In some patients with PD there are nonspecific alterations in the EEG, which nevertheless sometimes involve pathology. The presence of personality disorders along with JME has been repeatedly described. Previous studies have emphasized the difficulties in treating patients with JME, which have been attributed to some specific psychiatric, psychological and psychosocial characteristics.
ObjectivesDescribing distinctive personality traits in JME
MethodsReview of scientific literature based on a relevant clinical case.
Results19-year-old woman, single. Psychiatric history since she was 12 due to anxiety-depressive symptoms, after being diagnosed with JME. 4 admissions in Psychiatry, with a variety of diagnoses: eating disorder, attention deficit hyperactivity disorder and borderline personality disorder. The evolution of both disorders has been parallel, presenting epileptic seizures due to irregular therapeutic adherence together with pseudo-seizures, which made difficult their differential diagnosis. In addition, he has had frequent visits to the emergency room for suicide attempts and impulsive behaviors.
ConclusionsIn 1957, for the first time, distinctive personality traits were described in patients with JME: lack of control and perseverance, emotional instability, variable self-concept and reactive mood, which have been confirmed in subsequent studies. It is believed as epilepsy progresses, patients tend to develop symptoms of depression, anxiety, social problems, and attention deficit. Therefore, these patients have difficulty in following medical recommendations, especially precautions regarding precipitating factors for seizures.
DisclosureNo significant relationships.
Depressive Symptoms and Suicidal Ideation in Spanish Medical Students
- J.A. Blanco, M. Rodriguez, I. Santos Carrasco, M. Queipo De Llano De La Viuda, L. Gallardo Borge, P. Marqués Cabezas, M.J. Mateos Sexmero, J. Blanco Vilches
-
- Journal:
- European Psychiatry / Volume 65 / Issue S1 / June 2022
- Published online by Cambridge University Press:
- 01 September 2022, p. S183
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Medical students have higher rates of depression, anxiety and suicidal ideation over the general population. The onset of these disorders can be a risk factor with unfavorable impact in both medical care and their lives during the years of clinical specialization
ObjectivesTo assess the prevalence and factors involved in depression, anxiety and suicidal behavior in medical students of the University of Valladolid (Spain). The results are compared with a previous study conducted 5 years earlier
MethodsWe used an online self-administered questionnaire that included demographic variables, academic information, sanitary data, Beck Depression Inventory (BDI), Generalized Anxiety Disorder 7 (GAD7), and MINI International Neuropsychiatric Interview for suicide. Chi-Square Test was used for categorical variables, Student`s t-test for quantitative variables and Spearman’s Coefficient to evaluate correlations between variables
Results362 students of all courses enrolled in Medicine at the University of Valladolid completed the survey. There were no differences between male and female students, both with high rates of moderate-severe depression (27% vs 30,4%), anxiety (42,9% vs 54,5%), and moderate-severe suicide risk (14,2% vs 10,7%). Previous study (n=584) also showed no differences between sexes but with lower rates of moderate-severe depression (14,3% vs 16,3%). 11% reported suicidal thoughts in the past month (11,6% previous study). There was a significant inverse correlation between medical career satisfaction and BDI scores
ConclusionsFive years later, rates of depression and suicide risk could have increased in medical students at the University of Valladolid. We urgently recommend the implementation of mental health prevention programs in this population
DisclosureNo significant relationships.
Idiopathic serontonin syndrome. Can we prevent it?
- L. Gallardo Borge, I.D.L.M. Santos Carrasco, P. Marqués Cabezas, L. Rodriguez Andrés, A. Rodriguez Campos
-
- Journal:
- European Psychiatry / Volume 65 / Issue S1 / June 2022
- Published online by Cambridge University Press:
- 01 September 2022, p. S724
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Serotonin syndrome is a mild to potentially life-threatening syndrome associated with excessive serotonergic activity within the central nervous system. Serotonin syndrome is associated with medication use, drug interactions and overdose. All drugs that increase central serotonin neurotransmission at postsynaptic 5-HT1A and 5-HT 2A receptors can produce SS.
ObjectivesClinical case and literature review.
MethodsA 74-year-old female, married, diagnosed of major depressive disorder. Treated with: lithium 600 mg, quetiapine 50 mg, venlafaxine 300 mg. The doses had been maintained for the last months. Lithium levels in the normal range.
ResultsIn an emergency room, she received a tramadol injection because of strong backpain. After a few hours, she felt an overall worsening, sleepiness and lack of response to external stimuli. Given the persistence of the symptoms and decreased appetite along with decreased water intake, she attended to Hospital. She had a high fever, rigidity and myoclonus. Her language was incoherent. Blood tests showed high CK, and high AST and ALT.
ConclusionsSS is a potentially fatal iatrogenic complication of serotonergic polypharmacy. Considered idiopathic in presentation, it appears tipically after initiation or dose escalation of the offending agent to a regimen including other serotonergic agents. While serotonin syndrome is often associated with the use of selective serotonin inhibitors (SSRI), an increasing number of reports are being presented involving the use of tramadol. It is vital that clinicians are aware of the potential for SS when psychotropic and non-psychotropic agents are co-administered to certain patients, such as those with both depression and pain.
DisclosureNo significant relationships.
Monitoring sertraline and clozapine levels
- A. Rodriguez Campos, L. Rodriguez Andrés, G. Medina Ojeda, I. Santos Carrasco, J. Gonçalves Cerejeira, A. Gonzaga
-
- Journal:
- European Psychiatry / Volume 65 / Issue S1 / June 2022
- Published online by Cambridge University Press:
- 01 September 2022, p. S718
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
One of the most frequent side effects seen when prescribing sertraline and clozapine together is the appearance of a seizure crisis. This event is usually related to an increase of plasmatic concentration due to interactions of these drugs with blood components.
ObjectivesTo investigate the effects of clozapine when combined with other drugs, especially its effects increasing plasmatic concentration.
MethodsA patient was treated sith 300 mg/day of clozapine followed by a treatment with sertraline 50 mg/day, which increases plasmatic concentration. The combination of these treatments produced seizures. Other works published about interactions are reviewed.
ResultsIt is important to monitor clozapine dosages to avoid increasing plasmatic concentration, especially if other drugs that have this effect are also administered.
ConclusionsIt is important to monitor clozapine dosages to avoid increasing plasmatic concentration, especially if other drugs that have this effect are also administered.
DisclosureNo significant relationships.
Testosterona and suicide
- L. Gallardo Borge, I.D.L.M. Santos Carrasco, P. Marqués Cabezas, A.I. Segura Rodríguez, G. Medina Ojeda
-
- Journal:
- European Psychiatry / Volume 65 / Issue S1 / June 2022
- Published online by Cambridge University Press:
- 01 September 2022, p. S842
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Testosterone is an anabolic androgenic steroid hormone involved in brain development, reproduction, and social behavior. Several studies have shown that testosterone can cause impulsivity in humans. This impulsivity could modify the mood and increase the risk of suicidal behaviour.
ObjectivesTestosterone is an anabolic androgenic steroid hormone involved in brain development, reproduction, and social behavior. Several studies have shown that testosterone can cause impulsivity in humans. This impulsivity could modify the mood and increase the risk of suicidal behaviour.
MethodsClinical case and literature review.
ResultsA 33-years male (biological female), single, gypsy ethnicity, with an 11-years daughter. Psychiatric history of one admission in a hospitalization unit. Diagnosed of depressive disorder and personality disorder NOS. Intermittent follow-up in Mental Health consultations. 8 years later, he consulted due to gender dysphoria. He refered not to be feeling identified with his body for a long time. He rejected his sexual characteristics. After his mental evaluation, he was refered to Endocrinology Service. He had been prescribed with testosterone. Three days after starting the treatment, he maked anattempt of suicide with medication. The patient had not presented previous suicide attempts or ideation. With the withdrawal of the testosterone, the suicidal behaviour dissapeared.
ConclusionsDue to the association of testosterone and suicidal behavoiur, we consider that is important to pay attention to people who have just started the androgenic treatment in order to avoid a high risk of suicide. In the same way, we should focus on evaluating the hostility, impulsivity and irritability in patients strongly related to suicidal behaviour.
DisclosureNo significant relationships.
Voices change my name
- C. Vallecillo Adame, T. Jiménez Aparicio, C. De Andrés Lobo, A. Gonzaga Ramírez, M. Queipo De Llano De La Viuda, G. Guerra Valera, I. Santos Carrasco, J. Gonçalves Cerejeira, B. Rodríguez Rodríguez, M. Fernández Lozano, M.J. Mateos Sexmero, N. Navarro Barriga, N. De Uribe Viloria, G. Medina Ojeda, L. Rodriguez Andrés
-
- Journal:
- European Psychiatry / Volume 65 / Issue S1 / June 2022
- Published online by Cambridge University Press:
- 01 September 2022, p. S801
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
We present the clinical case of a patient where the psychotic clinic coexists with gender dysphoria. This scenario can be the result of a change in gender identity derived from the psychotic process or appear independently of it.
ObjectivesWe want to explain the importance of knowing how to act with a patient in whom these two processes coexist.
Methods20-year-old woman, with no history of mental health. She comes to the emergency department for behavioral alteration. The family observes strange behaviors, unmotivated laughter, soliloquies and aggressive episodes. Abandonment of studies, hobbies and radical physical change. Delusions of prejudice and self-referential delusions. Possible phenomena of echo and diffusion of the thought. Auditory hallucinations talking to her in male gender, since then she presents doubts about her sexual identity and manifests her desire to change sex. Altered judgment of reality.
ResultsDuring admission, we started treatment with an antipsychotic with good tolerance and she was referred to mental health team, where psychopharmacological treatment was adjusted with good response. In the following medical appointments the psychotic clinic disappeared at the same time that sexual identification was completely restored and made a critique of the behavior and experiences.
ConclusionsThis case highlights the importance of assessing the chronology of symptoms, the patient’s criticality, the response to antipsychotic treatment and the need to exclude the psychotic background of the desire for gender reassignment before making a therapeutic decision.
DisclosureNo significant relationships.
The Impact of Natural Hazards on Older Adult Health: Lessons Learned From Hurricane Maria in Puerto Rico
- Elizabeth L. Andrade, Megan Jula, Carlos E. Rodriguez-Diaz, Lauren Lapointe, Mark C. Edberg, Maria I. Rivera, Carlos Santos-Burgoa
-
- Journal:
- Disaster Medicine and Public Health Preparedness / Volume 17 / 2023
- Published online by Cambridge University Press:
- 02 November 2021, e52
-
- Article
- Export citation
-
Objective:
With natural hazards increasing in frequency and severity and global population aging, preparedness efforts must evolve to address older adults’ risks in disasters. This study elucidates potential contributors to the elevated older adult mortality risk following Hurricane Maria in Puerto Rico through an examination of community stakeholder preparedness, response, and recovery experiences.
Methods:In April 2018, qualitative interviews (n = 22) were conducted with stakeholders in 7 Puerto Rican municipalities. Interview transcripts were deductively and inductively coded and analyzed to identify salient topics and themes representing participant response patterns.
Results:The hurricane’s detrimental impact on older adult health emerged as a prominent finding. Through 6 months post-hurricane, many older adults experienced unmet needs that contributed to declining physical and emotional health, inadequate non-communicable disease management, social isolation, financial strain, and excess morbidity and mortality. These needs were predominantly consequences of lengthy public service gaps, unsafe living conditions, interrupted health care, and the incongruence between preparedness and event severity.
Conclusions:In a landscape of increasing natural hazard frequency and magnitude, a pattern of older adult risk has become increasingly clear. Study findings compel practitioners to engage in natural hazard preparedness planning, research, and policy-making that considers the multiple facets of older adult well-being.
Early changes in brain structure, functional connectivity and neuropsychiatric symptoms after HCV infection cure with direct-acting antivirals
- M. Cavero, Z. Mariño, R. Navines, J. Pariente, E. Muñoz Moreno, C. Bartres, L. Nacar, S. Lens, S. Rodriguez-Tajes, S. Cañizares, N. Bargallo, X. Forns, R. Martin-Santos
-
- Journal:
- European Psychiatry / Volume 64 / Issue S1 / April 2021
- Published online by Cambridge University Press:
- 13 August 2021, p. S254
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Hepatitis C virus (HCV) infection is known to be associated with neuropsychiatric manifestations as part of the disease. Previous neuroimaging studies showed brain connectivity dysfunction among HCV-infected patients
ObjectivesTo assess, by MR in resting state, the potential structural and connectivity changes before (BL) and after HCV eradication (FU12) with direct-acting antivirals (DAA), along with clinical parameters.
MethodsTwenty-one HCV-patients, aged≤55 years, without psychiatric history, nor advanced liver disease, and eligible for DAA, and 25 healthy controls were included. Evaluations were performed at BL and FU12. Brain volume and local gyrification index (LGI) were assessed in MR-T1, and functional connectivity by seed-based analysis (left insula). Depression (MADRS/PHQ9) and neurotoxicity symptomatology (NRS) were assessed. We compared patients between BL/FU12, and controls by means of paired/independent T-test analysis.
ResultsSubstained virologycal response was obtained in all patients (100%). Depressive and neurotoxicity symptomatology improved after cure (p<0.01). HCV-patients showed a reduced volume in a right latero-occipital area compared to controls (CWP<0.005) in both BL and FU12. This difference was smaller between FU12 and controls. LGI was higher in FU12-HCV compared to BL-HCV. fMRI connectivity showed a high association between insula and occipital/parietal territories in patients than controls, being higher among BL-HCV and controls. Differences were limited to occipital areas among FU12-HCV and controls.
ConclusionsNeuropsychiatric symptomatology improved after cure. Left insula is altered among HCV-patients in structured and connectivity (mainly occipital areas). After cure differences with controls were reduced, suggesting a partial restoration of brain connectivity.
The mediating role of impulsivity in the relationship between suicidal behaviour and early traumatic experiences in depressed subjects
- F. Dal Santo, J.J. Carballo, Á. Velasco, L. Jiménez-Treviño, J. Rodríguez-Revuelta, C. Martínez-Cao, I. Irene Caro-Cañizares, L. De La Fuente-Tomás, I. Menéndez-Miranda, L. González-Blanco, M.P. García-Portilla, J. Bobes, P.A. Saiz
-
- Journal:
- European Psychiatry / Volume 64 / Issue S1 / April 2021
- Published online by Cambridge University Press:
- 13 August 2021, p. S583
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Depressed patients with early traumatic experiences may represent a clinically distinct subtype with worse clinical outcome. Since early traumatic experiences alter the development of systems that regulate the stress response, certain personality features may influence coping strategies, putting individuals with depression and a history of early traumatic experiences at greater risk of suicidal behaviour.
ObjectivesTo determine whether impulsivity mediates the relationship between early traumatic experiences and suicidal behaviour in patients with major depressive disorder (MDD).
MethodsThe sample included 190 patients [mean age (SD)=53.71 (10.37); females: 66.3%], with current MDD. The Childhood Trauma Questionnaire-Short Form (CTQ-SF), the List of Threatening Experiences (LTE), and the Barratt Impulsiveness Scale-11 (BIS-11) were used to assess childhood and adulthood adverse life events and impulsivity. We developed mediation models by bootstrap sampling methods.
Results81 (42.6%) patients had previous suicide attempts (SA). CTQ-SF-Total and BIS-11-Total scores were higher in MDD patients with previous SA. Correlation analyses revealed significant correlations between the CTQ-SF-Total and BIS-11-Total, CTQ-SF-Total and HDRS-Total, and BIS-11-Total and HDRS-Total scores. Regression models found that CTQ-SF-Total, BIS-11-Total, and HDRS-Total scores were associated with SA. Mediation analyses further revealed the association between CTQ-SF-Total and SA was mediated by the indirect effect of the BIS-11-Total score (b=0.007, 95% CI=0.001, 0.015), after controlling for sex, HDRS-Total, and LTE-Total.
ConclusionsImpulsivity could mediate the influence of childhood trauma on suicidal behaviour. This will help understand the role of risk factors in suicidal behaviour and aid in the development of prevention interventions focused on modifiable mediators when risk factors are non-modifiable.
Association of traumatic events in childhood, impulsivity and decision-making with previous suicide attempt and/or current suicidal ideation in adult patients with major depressive disorder
- A. Roman, J. Rodríguez-Revuelta, F. Dal Santo, L. García-Alvarez, L. De La Fuente-Tomás, C. Martínez-Cao, L. Jiménez-Treviño, L. González-Blanco, M.P. García-Portilla, J. Bobes, P.A. Saiz
-
- Journal:
- European Psychiatry / Volume 64 / Issue S1 / April 2021
- Published online by Cambridge University Press:
- 13 August 2021, pp. S177-S178
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Suicidal behavior has a great impact on world public health. The literature describes the possible existence of an association between neurobiological, clinical and cognitive factors in suicidal behavior.
ObjectivesTo determine the possible relationship between clinical variables (history of abuse/maltreatment in childhood), psychopathology (impulsivity traits) and cognitive (decision-making) with a history of suicide attempt and/or current suicidal idea in patients with major depressive disorder.
MethodsCross-sectional study in a sample of adult patients with major depressive disorder in which two types of comparisons are made. In the first case, two groups were compared based on the presence or absence of history of suicide attempt. In the second case, two groups were compared based on the presence or absence of suicidal ideation in the same sample of patients. Finally, sociodemographic, clinical and cognitive variables were evaluated in that population sample.
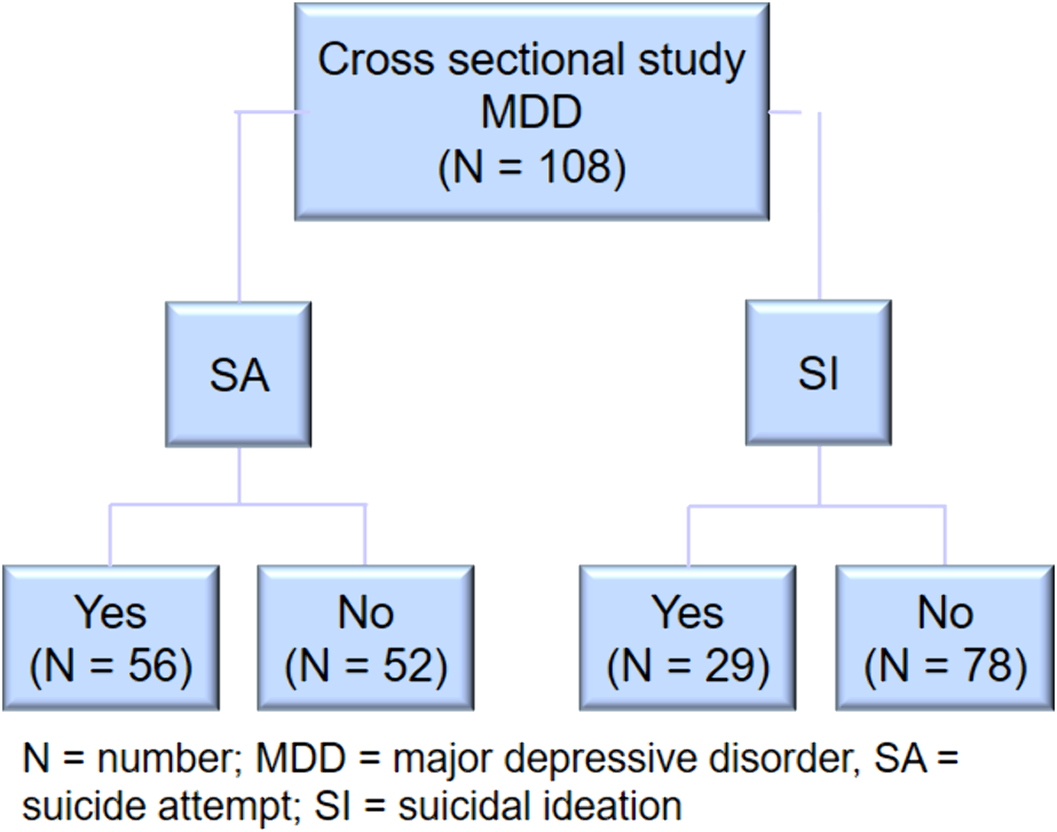 Results
ResultsWhen the joint influence of sociodemographic, clinical and cognitive characteristics are present, it can be said that being single/divorced/separated, a history of sexual abuse in childhood and an alteration in decision-making, specifically a lower number of choices of deck D in the IGT test, are associated with a higher probability of a personal history of suicide attempt. While a higher score on the Barrat impulsivity scale is associated with a greater probability of presenting current suicidal ideation once the influence of sociodemographic, clinical and cognitive variables has been taken into account.
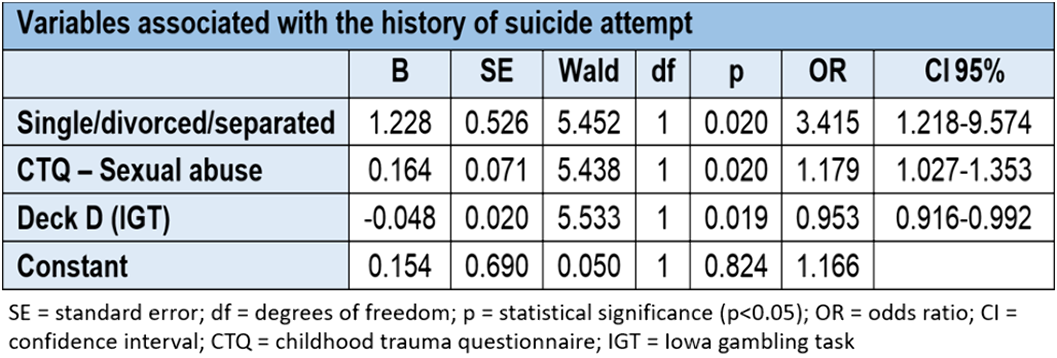
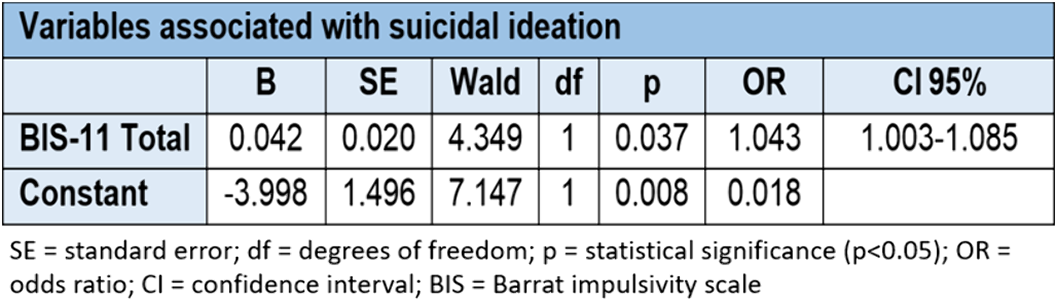 Conclusions
ConclusionsDifferent sociodemographic, clinical and cognitive factors are associated with the presence of a history of suicide attempt and/or current suicidal ideation.
DisclosureNo significant relationships.
“Covid madness”
- C. Capella Meseguer, E. Rodríguez Vázquez, J. Gonçalves Cerejeira, I. Santos Carrasco, L. García García
-
- Journal:
- European Psychiatry / Volume 64 / Issue S1 / April 2021
- Published online by Cambridge University Press:
- 13 August 2021, p. S297
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
We present the case of a man who, after receiving treatment for Covid-19 pneumonia, suffers a manic episode induced by medication.
ObjectivesThis case is chosen to present as an example of a psychiatric illness derived from Covid-19, in this case secondary to its treatment.
MethodsWe present a manic episode induced by covid medication.
ResultsComplementary examinations are carried out in which organic pathology is ruled out, being diagnosed of a manifest episode in probable relation to the treatments used and hospital admission is decided due to the impossibility of home management. Neuroleptic and anxiolytic treatment was started at low doses with a good response, and he was discharged with complete recovery and critiqued of the episode.
ConclusionsIt is estimated that between 20-40% of patients with COVID infection have presented neuropsychiatric symptoms. Mania secondary to treatment was reported in 13 (0 · 7%) of 1744 patients with coranavirus included in a study (1). The Spanish Pharmacivigilance System of Medicines for Human Use (SEFV-H) closely monitors the suspected adverse reactions reported with drugs considered potential therapeutic strategies for SARS-CoV-2 infection. 327 cases of adverse reactions have been reported, of which 18 cases include 28 thermal cases of suspected psychiatric adverse reactions. The interest of this case lies in the fact that it illustrates a psychiatric disorder derived from Covid-19, in this case secondary to the treatment used, which causes a manifest episode with a typical evolution in this type of case with rapid improvement at low doses of antipsychotics.







